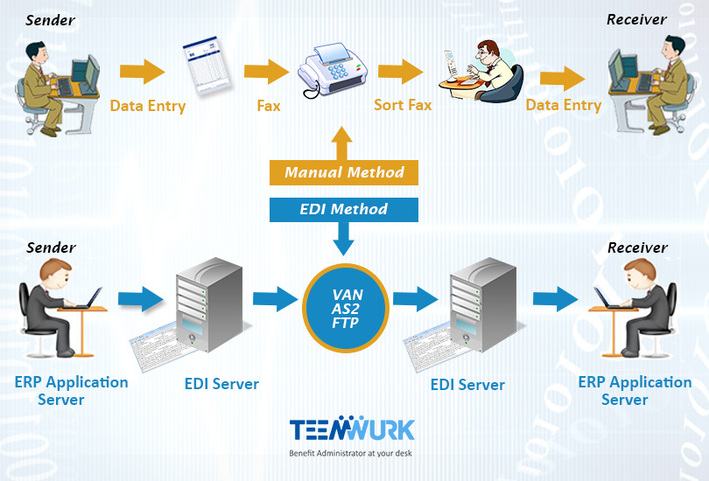
The key benefits enrollment and administration transactions, termed as EDI 834 transactions are to be made in strict compliance with HIPAA specifications. The transactions are critical for the benefits administration processing that includes new enrollments, editing and restoration of existing enrollments and termination of ex-employee enrollments.
Every EDI document is the specific one and contains every individual subscriber’s personal and demographic information, healthcare eligibility, plan network and reference information. Once the administrator enters the required information, the files are further transmitted to the respective carriers.
These transactions may or may not involve TPAs (third party administrator) who facilitate the process by helping employers to encrypt data as per recipient specifications. Usually, employers associate with service providers who can help them execute the benefits administration process efficiently. Every insurance carrier, with a view to keep the confidentiality of the information intact, put certain specifications that require slight amendments to be made in the standard format. But, around 95% service providers transmit files in generic 834 format and thus, face trouble while sending files to carriers as they are not carrier-specific and carrier systems don’t accept files in generic formats.
This discrepancy in data file transmission not only wastes critical time but also delays the enrollment processing on the whole. The Robust EDI tool offered by TeemWurk can help you perform employee benefits administration tasks effectively and can make required amendments in your file formats as per carrier specifications.
Therefore, the solution can provide you generic 834 as well as customized 834 documents according to the carrier-specific needs and requirements. The process is not only time and cost effective, but will allow you to ensure error-free data transmissions.
Every EDI document is the specific one and contains every individual subscriber’s personal and demographic information, healthcare eligibility, plan network and reference information. Once the administrator enters the required information, the files are further transmitted to the respective carriers.
These transactions may or may not involve TPAs (third party administrator) who facilitate the process by helping employers to encrypt data as per recipient specifications. Usually, employers associate with service providers who can help them execute the benefits administration process efficiently. Every insurance carrier, with a view to keep the confidentiality of the information intact, put certain specifications that require slight amendments to be made in the standard format. But, around 95% service providers transmit files in generic 834 format and thus, face trouble while sending files to carriers as they are not carrier-specific and carrier systems don’t accept files in generic formats.
This discrepancy in data file transmission not only wastes critical time but also delays the enrollment processing on the whole. The Robust EDI tool offered by TeemWurk can help you perform employee benefits administration tasks effectively and can make required amendments in your file formats as per carrier specifications.
Therefore, the solution can provide you generic 834 as well as customized 834 documents according to the carrier-specific needs and requirements. The process is not only time and cost effective, but will allow you to ensure error-free data transmissions.

 RSS Feed
RSS Feed
